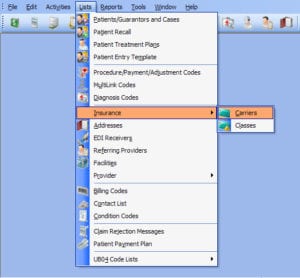
To access the Insurance Carrier List, go to Lists, then Insurance, then Carriers OR click on the Insurance Carrier List speed button on the toolbar (with the blue + sign).
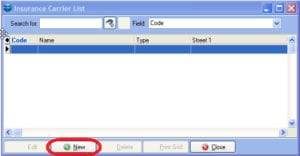
Click on New to set up a new payer in the system.
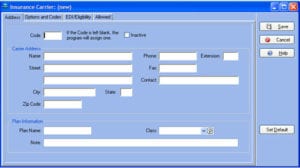
For our Medisoft Network providers, at time of initial setup Medical Billing Professionals will set up your Blue Cross Blue Shield, Medicare and Medicaid payers on your Insurance Carrier list for you. However, you are responsible for setting up all other insurance payers. Therefore, it is important for you to know if a payer accepts claims electronically or not.
At the time of initial setup, MBP will set up your insurance carrier list so that all carriers you enter by default will be to go electronic through our clearinghouse/EDI Receiver.
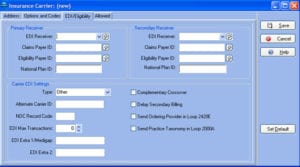
If the payer DOES accept electronically, you will have to enter the Payer ID number in the EDI Payor Number field of the EDI tab of the insurance carrier setup.
- Providers should always refer to the payer lists available on our websites. You can search by insurance carrier name or by EDI Payer number. There are 2 separate lists–Commercial Payer List and Government Payer List (for Blue Cross Blue Shield, Medicare and Medicaid payers).
- If the payer does NOT accept electronically, you will want to change the default billing method on the Options tab of the Insurance Carrier setup from Electronic to Paper. Then, on the EDI Codes tab, you will want to delete MD On-Line as the EDI Receiver and leave that field blank.
- If MBP is sending your paper claims and the Default Billing Method is paper, you must enter the payer’s fax number in the system.
- NOTE: For payers that do NOT accept electronic claims, MBP can send claims on paper through the Clearinghouse Print Service. If you choose this option, the Default Billing Method must be Electronic and the EDI Receiver must be MD On-Line. In addition, the Payer ID number is SPRNT.
- It is VERY important when setting up an insurance payer in the system that you list a complete mailing address (street address, city, state and zip). Do NOT just enter the payer name, even if the payer accepts electronically.
- For payers that DO accept electronically, it is only necessary to set up one payer in the system for each insurance carrier.
- For example, Aetna has different claim offices throughout the country. However, because claims are routed to the same Payer ID number, you only set up one Aetna payer in the system. Don’t worry if your payer setup has, for example, a mailing address in Blue Bell, PA, but the address on the card for claims is in El Paso, TX.
- This applies for all insurance companies. Most providers will only have one Blue Cross Blue Shield set up in their system. It is important to remember that claims are NOT sent to out-of-state Blue Cross Blue Shield plans, but to your local plan. Do NOT set up multiple Blue Cross Blue Shield payers in your system, unless you participate with the out-of-state plan.


Recent Comments